Introduction and Parts 1 & 2
My Alice-In-Wonderland-rabbit-hole moment came after time off from work in Summer 2021. At this time discussions regarding herd immunity were called into the mainstream again, in the wake of a “successful” vaccination campaign. A certain percentage of the population being vaccinated could open the country and allow a return to normalcy. Smallpox, poliovirus, and measles vaccines were mentioned in passing, as though these diseases and conditions were similar. It was at this point I had to call bullsh**.
We had been led to believe since Spring of 2020 that we could “end this pandemic,” which they insinuated meant that we could eradicate it. This message was repeated constantly, often in conjunction with messages both appealing to our altruistic natures and stirring fear, and by high-level medical “experts” and elected officials alike. The public was shown this carrot every chance they could— that there existed a post-pandemic world where SARS-CoV-2 had disappeared. We could win and the virus could lose. Like wars past, the war on drugs, the war on terror, now the war on COVID-19. These political platitudes had no legitimacy being anywhere near this situation. Yet, even supposed medical “experts” jumped in this game, deviating from established scientific principles on which public health, epidemiology, and virology are based. So the “noble lie” began. Or further evolved.
Back to summer 2021, I set out to delineate where truth began and their misinformation ended, starting with herd immunity and RNA viruses. Armed with freshly purchased textbooks- The Principles of Virology: Volumes 1 & 2 and Gordis Epidemiology (copyrights 2020 & 2019, respectively)- I got to truth-seeking. Onward, down the rabbit hole.
Herd Immunity Definition
Herd immunity refers to the presence of protective immunity (naturally-acquired OR vaccine-induced) in a portion of the population that is sufficient to impede person-to-person transmission. Decreased spread means those that are not yet immune can be protected. For herd immunity to exist, certain conditions must be met:
1. Transmission occurs only within a single host species.
2. Transmission must be relatively direct from one member of a population to another.
3. Infections and/or vaccinations must induce solid immunity— partial immunity will not allow herd immunity to operate.1 2
LIE 1: Ignoring the significance of interspecies transmission
Requirement #1 means that a virus can only circulate within our human species to allow herd immunity to be possible. If an alternative reservoir or intermediate host exists, the virus can hide out, circulate, and mutate within these other species, biding its time until a susceptible human is exposed, thereby subsequently allowing spread among humans once again. So goes the cycle, with spread then back to the reservoir/intermediate host, and then back to humans again. You can imagine that the overlapping circles of transmission might get so bad as to resemble a Spirograph picture. These types of infection cycles, especially for respiratory infections, make controlling the spread much like Whack-A-Mole. Aims for eradication are rife with hubris and simply are unattainable in the longterm (hence requirement #1).
We have been told nearly since the start of the pandemic that this virus arose from bats. Whether this, the lab leak scenario, or some other event is true, so long as bat transmission is possible, we by definition could never expect herd immunity to occur as they were implying. In fact, SARS-CoV-2 has been identified in multiple species. A few examples include minks, cats, dogs, ferrets, and recently deer.3 4 5 And in mid-2020, the possible first variant of interest (due to the presence of multiple spike mutations) was discovered circulating among humans and farmed minks.6 This is a perfect illustration of how SARS-CoV-2 can and will continue to evolve and persist throughout the world. And remember the ample discussion in spring of 2020 regarding transmissibility to our pets? Plus it’s been known for years (since ~2003 and 2012, respectively) that the closely related viruses SARS-CoV and MERS-CoV are zoonoses.
Bottom line: Condition #1 for herd immunity cannot be achieved. And it was publicly known since nearly day one.
LIE 2: Vaccines are the only way out; discounting natural immunity or cross-immunity
You may have noticed that the above definition of herd immunity includes both naturally-acquired and vaccine-induced. Wow, so did our “experts” somehow forget Virology, Immunology, and Epidemiology 101? “Vaccines that mimic the natural infection” are considered to be among the most “extraordinary” achievements in medical history.7 Vaccine-induced immunity attempts to recapitulate the response that occurs with natural immunity, ergo natural immunity is the standard being attempted. From a vaccinology textbook8:
“In order to achieve immunity by vaccination, a vaccine has to be able to emulate the immunogenic components of natural infection without causing the disease.”
The immune response to natural infection is the fundamental basis for vaccine development. But vaccine-induced immunity often times falls short, among one of the many reasons that vaccine development can take decades.9 10 Such has been the highly relevant example of SARS-CoV and MERS-CoV vaccine candidates. From a 2020 publication summarizing the results of a MERS vaccine human clinical trial11:
“The development of MERS vaccine candidates has been challenging because the determinants of protective immunity remain incompletely understood.”
The immune response is complex and artificially recreating it can lead to many unforeseen challenges and findings. So how and why are so many of these “experts” now stating that natural immunity is inferior to the induced immunity which is based on natural immunity?
It’s kind of like:
Pretending that natural immunity is somehow substandard is an oxymoron. It’s the pitch of a snake-oil salesman. Buyer beware.
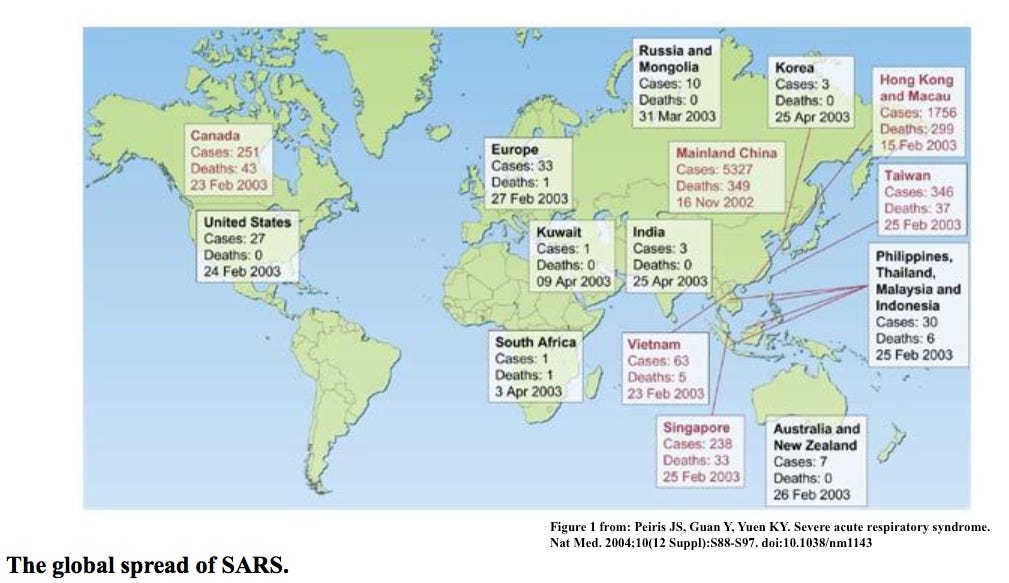
With regard to natural immunity, lessons from SARS-CoV can be instructional, despite it never getting close to the scale of SARS-CoV-2 pandemic. Through their analysis of SARS-CoV, they found that its mutation rate was similar to other RNA viruses (like SARS-CoV-2), but transmission was monumentally better contained (only over 8,000 cases (8,096 in one source) identified from the original outbreak), likely in large part due to its lower transmissibility.12 13 14
Consequently the number of variants identified was also drastically lower (only several dozen, perhaps up to ~100).15 16 17 18 Immune response after SARS-CoV infection has been shown to persist for many years. Studies investigating the durability of humoral (antibody) responses have shown that they may wane as little as 2-3 years post-infection but can remain detectable for up to 6 years.19 20 T-cell mediated immunity has been shown by many studies to endure for 6, 11, and up to 17 years (depending on time elapsed from infection based on the year of study publication).21 22 23 24 This gives credence to the argument for the durability of natural immunity against SARS-CoV-2, even if at some point due to more divergent variants arising, infections may occur.
There’s also the topic of cross-immunity or cross-protection. This type of immunity develops from exposure to one pathogen but also provides some degree of future immunity to related strains or even unrelated pathogens as well. This is the very basis of Dr. Edward Jenner’s infamous discovery- using cowpox virus to induce immunity to the related smallpox virus. It remains the basis of existing smallpox vaccines which use vaccinia, another related poxvirus most closely related to horsepox virus, and the widely used Bacillus Calmette−Guérin (BCG) vaccine for tuberculosis, which uses a cow strain (Mycobacterium bovis) related to the etiologic bacterium for TB (Mycobacterium tuberculosis).25 26
In spring of 2020 it was suggested that cross-immunity from other coronaviruses, such as those that caused the common cold in previous years, might be possible. A completely logical theory based on previous scientific knowledge. For example, during a 2018 clinical trial for one MERS-CoV vaccine candidate (NCT03399578)27, researchers found that prior to being given the vaccine, a handful of participants (4/24) had positive antibody or T-cell responses to MERS-CoV despite never having MERS. They concluded it was likely due to exposure to common coronaviruses, such as HCoV-229E, HCoV-HKU1, HCoV-NL63, and HCoV-OC43, circulating worldwide in years prior. They cited a prevalence study which found that 100 % of children in the Netherlands had seroconverted to at least one of these by the age of 10 years, a rate they said is likely present in other countries.
Yet this highly important topic in the midst of a pandemic was quickly forgotten in mainstream discussion soon after it was stated. After all it might dampen fears in the minds of the masses.
However, recent SARS-CoV-2 studies have confirmed that cross-immunity from common cold coronaviruses does exist28 29 30 and may help to explain the asymptomatic or mild cases in some people, especially children.31 From a study published July 2020, T cells from those who recovered from SARS-CoV 17 years prior displayed strong cross-reactivity to the nucleocapsid (N) protein of SARS-CoV-2. Additionally they found SARS-CoV-2-specific T cells in individuals with no history of SARS, COVID-19, or contact with individuals who had SARS and/or COVID-19. These findings suggest that infection with betacoronaviruses (SARS-CoV, SARS-CoV-2, or common cold viruses) “induces multi-specific and long-lasting T cell immunity against the structural N protein.”
Other sources of cross-immunity have been investigated as well. It has been suggested that the BCG tuberculosis vaccine commonly administered in countries outside of the U.S. may confer some degree of cross-immunity.32 Other recent studies suggest there may be some cross-immunity from having received the IPV (inactivated poliovirus), MMR (measles, mumps, rubella), or Tdap (tetanus, diphtheria, pertussis) vaccines.33 34 Seeing as how children receive several doses over their early years, this could also help to explain their milder infections.
Bottom line: Multiple modes of acquired immunity can help to decrease case numbers and decrease severity of illness. The COVID-19 vaccines are not needed as a broad, sweeping solution for all, everywhere (and for many reasons other than just from this perspective).
*NOTE: Parts 3-7 & Conclusion to follow soon. Rather than keep it as one long, dizzying piece, I decided (with some wise nudging) to divide it.
References:
Flint J, Racaniello VR, Rall GF, Hatziioannou T, Skalka AM. Principles of Virology. 5th ed. ASM Press; 2020.
Celentano DD, Szklo M. Gordis Epidemiology. 6th edition. Elsevier; 2019.
Meyerowitz EA, Richterman A, Gandhi RT, Sax PE. Transmission of SARS-CoV-2: A Review of Viral, Host, and Environmental Factors. Ann Intern Med. 2021;174(1):69-79. doi:10.7326/M20-5008. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7505025/
Maron DF. Wild U.S. deer found with coronavirus antibodies. National Geographic. Accessed online 8/6/2021. https://www.nationalgeographic.com/animals/article/wild-us-deer-found-with-coronavirus-antibodies
European Centre for Disease Prevention and Control. Detection of new SARS-CoV-2 variants related to mink – 12 November 2020. ECDC: Stockholm; 2020. https://www.ecdc.europa.eu/sites/default/files/documents/RRA-SARS-CoV-2-in-mink-12-nov-2020.pdf
Badgujar KC, Badgujar VC, Badgujar SB. Vaccine development against coronavirus (2003 to present): An overview, recent advances, current scenario, opportunities and challenges. Diabetes Metab Syndr. 2020;14(5):1361-1376. doi:10.1016/j.dsx.2020.07.022. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7371592/
Morrow, WJW; Sheikh, NA; Schmidt, CS; Davies, DH. Vaccinology: Principles and Practice. Wiley-Blackwell; September 2012.
Smatti MK, Al Thani AA, Yassine HM. Viral-Induced Enhanced Disease Illness. Front Microbiol. 2018;9:2991. Published 2018 Dec 5. doi:10.3389/fmicb.2018.02991. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6290032/
Song Z, Xu Y, Bao L, Zhang L, Yu P, Qu Y, Zhu H, Zhao W, Han Y, Qin C. From SARS to MERS, Thrusting Coronaviruses into the Spotlight. Viruses. 2019 Jan 14;11(1):59. doi: 10.3390/v11010059. PMID: 30646565; PMCID: PMC6357155. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6357155/
Koch T, Dahlke C, Fathi A, et al. Safety and immunogenicity of a modified vaccinia virus Ankara vector vaccine candidate for Middle East respiratory syndrome: an open-label, phase 1 trial. Lancet Infect Dis. 2020;20(7):827-838. doi:10.1016/S1473-3099(20)30248-6. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7172913/
Trovato M, Sartorius R, D'Apice L, Manco R, De Berardinis P. Viral Emerging Diseases: Challenges in Developing Vaccination Strategies. Front Immunol. 2020;11:2130. Published 2020 Sep 3. doi:10.3389/fimmu.2020.02130. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7494754/
Smatti MK, Al Thani AA, Yassine HM. Viral-Induced Enhanced Disease Illness. Front Microbiol. 2018;9:2991. Published 2018 Dec 5. doi:10.3389/fmicb.2018.02991. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6290032/
Hayashi T, Ura T, Abiko K, Mandan M, Yaegashi N, et al. Reasons why new coronavirus, SARS-CoV-2 infections are likely to spread. J Genet Med Gene Ther. 2020; 3: 001-003. https://www.heighpubs.org/jgmgt/pdf/jgmgt-aid1005.pdf
The Chinese SARS Molecular EpidemiologyConsortium. Molecular Evolution of the SARS Coronavirus During the Course of the SARS Epidemic in China. Science. 12 Mar 2004. Vol 303, Issue 664, p 1666-1669. DOI: 10.1126/science.1092002
Vega, V.B., Ruan, Y., Liu, J. et al. Mutational dynamics of the SARS coronavirus in cell culture and human populations isolated in 2003. BMC Infect Dis 4, 32 (2004). https://doi.org/10.1186/1471-2334-4-32 https://bmcinfectdis.biomedcentral.com/articles/10.1186/1471-2334-4-32#citeas
Xu D , Zhang Z, Wang FS. SARS-Associated Coronavirus Quasispecies in Individual Patients. N Engl J Med 2004; 350:1366-1367. DOI: 10.1056/NEJMc032421. https://www.nejm.org/doi/10.1056/NEJMc032421?url_ver=Z39.88-2003&rfr_id=ori:rid:crossref.org&rfr_dat=cr_pub%20%200www.ncbi.nlm.nih.gov
Inberg A, Linial M. Evolutional insights on uncharacterized SARS coronavirus genes. FEBS Letters. Volume 577, Issues 1–2. 2004. P 159-164.https://doi.org/10.1016/j.febslet.2004.09.076. https://www.sciencedirect.com/science/article/pii/S001457930401213X
Cao WC, Liu W, Zhang PH, Zhang F, Richardus JH. Disappearance of antibodies to SARS-associated coronavirus after recovery. N Engl J Med. 2007 Sep 13;357(11):1162-3. doi: 10.1056/NEJMc070348. PMID: 17855683.https://www.nejm.org/doi/pdf/10.1056/NEJMc070348
Tang F, Quan Y, Xin ZT, Wrammert J, Ma MJ, Lv H, Wang TB, Yang H, Richardus JH, Liu W, Cao WC. Lack of peripheral memory B cell responses in recovered patients with severe acute respiratory syndrome: a six-year follow-up study. J Immunol. 2011 Jun 15;186(12):7264-8. doi: 10.4049/jimmunol.0903490. Epub 2011 May 16. PMID: 21576510.
Oh H.L., Chia A., Chang C.X., Leong H.N., Ling K.L., Grotenbreg G.M. Engineering T cells specific for a dominant severe acute respiratory syndrome coronavirus CD8T cell epitope. J Virol. 2011;85(20 (October)):10464–10471. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3187484/
Ng OW, Chia A, Tan AT, et al. Memory T cell responses targeting the SARS coronavirus persist up to 11 years post-infection. Vaccine. 2016;34(17):2008-2014. doi:10.1016/j.vaccine.2016.02.063. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7115611/
Le Bert, N., Tan, A.T., Kunasegaran, K. et al. SARS-CoV-2-specific T cell immunity in cases of COVID-19 and SARS, and uninfected controls. Nature584, 457–462 (2020). https://doi.org/10.1038/s41586-020-2550-z. https://www.nature.com/articles/s41586-020-2550-z#citeas
Liu WJ, Zhao M, Liu K, et al. T-cell immunity of SARS-CoV: Implications for vaccine development against MERS-CoV. Antiviral Res. 2017;137:82-92. doi:10.1016/j.antiviral.2016.11.006. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7113894/
Jacobs BL, Langland JO, Kibler KV, et al. Vaccinia virus vaccines: past, present and future. Antiviral Res. 2009;84(1):1-13. doi:10.1016/j.antiviral.2009.06.006. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2742674/
Redelman-Sidi G. Could BCG be used to protect against COVID-19?. Nat Rev Urol. 2020;17(6):316-317. doi:10.1038/s41585-020-0325-9. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7184546/
Folegatti PM, Bittaye M, Flaxman A, et al. Safety and immunogenicity of a candidate Middle East respiratory syndrome coronavirus viral-vectored vaccine: a dose-escalation, open-label, non-randomised, uncontrolled, phase 1 trial [published correction appears in Lancet Infect Dis. 2020 May 12;:] [published correction appears in Lancet Infect Dis. 2020 Jun 8;:]. Lancet Infect Dis. 2020;20(7):816-826. doi:10.1016/S1473-3099(20)30160-2 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7172901/
Loyal L et al. Cross-reactive CD4+ T cells enhance SARS-CoV-2 immune responses upon infection and vaccination. Science. Vol 374, Issue 6564. https://www.science.org/doi/10.1126/science.abh1823
Goldman B. Stanford study ties milder COVID-19 symptoms to prior run-ins with other coronaviruses. Stanford Medicine News. July 1, 2021. Accessed online 10/2021. https://med.stanford.edu/news/all-news/2021/07/stanford-study-ties-milder-covid-19-symptoms-to-prior-run-ins-wi.html
Ng KW, Faulkner N, Cornish GH, et al. Preexisting and de novo humoral immunity to SARS-CoV-2 in humans. Science. 2020;370(6522):1339-1343. doi:10.1126/science.abe1107. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7857411/
Sagar M, Reifler K, Rossi M, et al. Recent endemic coronavirus infection is associated with less-severe COVID-19. J Clin Invest. 2021;131(1):e143380. doi:10.1172/JCI143380. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7773342/
Gonzalez-Perez M, Sanchez-Tarjuelo R, Shor B, Nistal-Villan E and Ochando J (2021) The BCG Vaccine for COVID-19: First Verdict and Future Directions. Front. Immunol. 12:632478. doi: 10.3389/fimmu.2021.632478
Comunale BA, Jackson-Ward E, Jiang Y, Ward LP, Liu Q, Ji L, Lai M, Engineer L, Comunale RA, Xie Q. Inactivated Poliovirus Vaccine Induces Antibodies that Inhibit RNA Synthesis of SARS-CoV-2: An open-label, pre-post vaccine clinical trial. medRxiv 2021.10.05.21264598; doi: https://doi.org/10.1101/2021.10.05.21264598.
Mysore V, Cullere X, Settles ML, Ji X, Kattan MW, Desjardins M, Durbin-Johnson B, Gilboa T, Baden LR, Walt DR, Lichtman AH, Jehi L, Mayadas TN. Protective heterologous T cell immunity in COVID-19 induced by the trivalent MMR and Tdap vaccine antigens. Med (N Y). 2021 Sep 10;2(9):1050-1071.e7. doi: 10.1016/j.medj.2021.08.004. Epub 2021 Aug 14. PMID: 34414383; PMCID: PMC8363466. https://pubmed.ncbi.nlm.nih.gov/34414383/